How studying protein expression can change the way we look at non-genetic diseases
By: Olivia Okubo Peviani
Alzheimer’s is one of the most devastating neurological disorders, and it still remains largely incurable, with current FDA-approved drugs only slowing down the progression of the disease when it comes to cognitive decline. This is because most if not all current treatments focus on targeting these protein fragments called amyloid-beta, which accumulates in the brain of Alzheimer’s patients.1 Not only do they not provide a cure or reverse the disease, but they can also cause amyloid-related imaging abnormalities (ARIA), a side effect that can lead to brain swelling (edema) and small brain bleeds known as microhemorrhages.2 Dr. Xian Chen’s goal is to directly investigate the molecular drivers of this disease: proteins. As Dr. Chen explains, “Proteins are the real executors of cellular function. They determine whether a cell is healthy or diseased.”
Figure 1. Picture of Dr. Xian Chen next to a mass spectrometry machine
DNA contains instructions which the RNA then carries and translates into protein. Many diseases, such as Alzheimer’s, happen at the protein level, which is why studying proteins can oftentimes be more informative than genetic typing alone.3 Dr. Chen’s lab focuses on not only the development but also the application of proteomics, which is the study of all proteins expressed in a cell or tissue. He also uses mass spectrometry in order to identify and quantify protein, which helps in determining whether or not the tissue/cell is diseased. Mass spectrometry helps with detecting changes in expression, modifications, and interactions when it comes to protein.3
Approximately 10 years ago, Dr. Chen’s lab developed a chemoproteomics approach, which is a technique scientists use to study proteins and how they interact with each other inside cells.4 Around most proteins work together, with interactions ranging from controlling each other’s activities, to forming pathways that can contribute to the behavior of a cell.5 By looking at one protein, it is like looking at one player on a team, while diseases such as Alzheimer's often arise from interactions between many proteins. As Dr. Chen explains, “We wanted to understand not just which proteins are present, but how they interact and contribute to disease progression.”
With this new information, Dr. Chen’s lab shifted their goal into understanding and identifying which protein actively drives Alzheimer’s progression, specifically looking at proteins that are abnormally active in a patient’s brain. That is when they discovered an epigenetic regulator called G9A. G9A is a protein that exists in many cells in the human body and normally plays a role in controlling gene activity.3 An epigenetic regulator is a protein that controls whether a certain gene is switched on or off. Rather than altering the DNA itself, it only modifies how the genes are expressed, which in turn influences how much of a particular protein. 6 This protein (G9A) normally silences gene expression, but in an Alzheimer's brain it becomes abnormally active, which then leads to an over-production of disease driving proteins. This happens because it interacts with the cellular machinery that produces proteins to promote harmful protein synthesis.3 This means that G9A is basically a “master switch”, so by inhibiting it, instead of focusing on one harmful protein, they would be able to reduce multiple proteins contributing to disease at once.
After figuring out what was driving Alzheimer’s, their goal shifted from discovery into production. If G9A drives pathology, the way to stop it is to inhibit it. One of the greatest challenges is that the human body has a blood-brain barrier that blocks any toxins from entering our brain. Therefore, although this could be helpful for preventing certain diseases, in this case, it is bad because it also blocks drug delivery.3 What they are now trying to figure out is how to design a drug small enough to cross the blood-brain barrier and reach the brain. The goal is to deliver it to the hippocampus, the region responsible for memory and learning, which is heavily affected in Alzheimer's disease.
They tested this new drug in three different Alzheimer’s mice models, and after the experiment they discovered that all of the mice showed signs of enhanced cognitive abilities, improved learning, memory, and an overall reversed disease pathology. Thus, unlike existing therapies, this specifically targets upstream mechanisms; in other words, instead of targeting the visible amyloid plaques, Dr. Chen’s approach focuses on interrupting the process that causes the damage in the first place. Therefore, by intervening earlier, we would be able to prevent the cascade entirely. As he puts it, “Most complex diseases occur at the protein level. If we can understand and control those changes, we open new therapeutic possibilities.”
Although these findings are promising, there are still many challenges that Dr. Chen’s lab must overcome before this approach can become an actual treatment for patients with Alzheimer's. Much of the current research being done has been tested in animals, but results in mice do not always equate to the same results in humans. In addition, epigenetic regulators such as the G9A can be hard to target due to them controlling the activity of many genes at one. If they are inhibited incorrectly, it could lead to problems in other cellular processes beyond the intended target. Another challenge is getting the drugs to safely cross the blood-brain barrier and for them to remain in the system long enough for it to take effect. This means that further research and clinical trials will be needed before Dr. Chen’s lab releases this strategy as treatment.
The next step is undergoing toxicity and safety testing and moving towards clinical trials so that they could potentially release this drug to the hospitals and so that it can be used as an actual Alzheimer’s treatment. Proteomics may reshape how we approach complex diseases beyond Alzheimer’s. Dr. Chen’s work is part of a broader shift toward functional biology, what once started as a question about which proteins drive Alzheimer’s has evolved into something that challenges the traditional boundaries set for diagnosis and therapy.
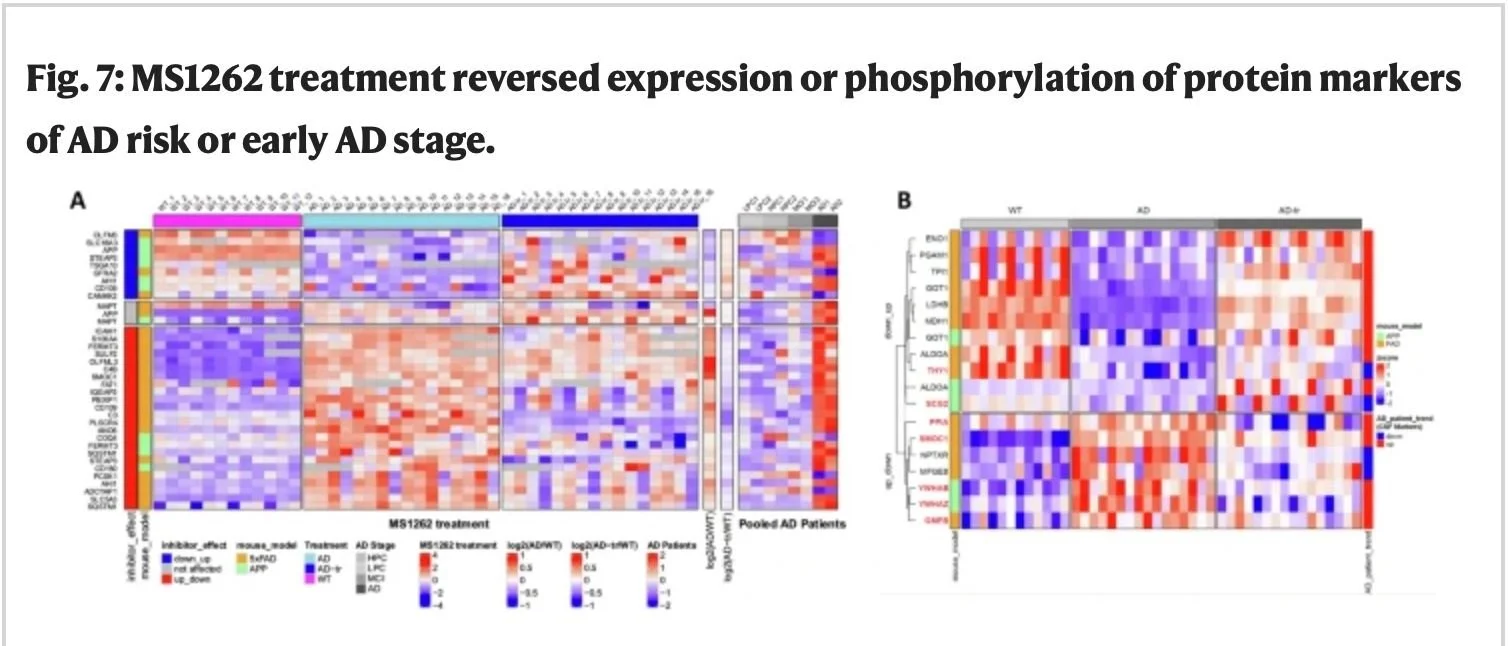
Figure 2. Figure showcasing data given by the mass spectrometry
References:
Mayo Clinic. Alzhei[RP1] mer’s disease: Symptoms & causes. Mayo Foundation for Medical Education and Research. https://www.mayoclinic.org/diseases-conditions/alzheimers-disease/symptoms-causes/syc-20350447 (accessed 2026-03-16).
National Center for Biotechnology Information. Probable lecanemab-associated pontine hemorrhage following anti-amyloid therapy.https://pmc.ncbi.nlm.nih.gov/articles/PMC12365432/ (accessed 2026-03-16).
Interview with Xian Chen, Ph.D. 2/24/26
Taylor & Francis. Chemoproteomics. https://taylorandfrancis.com/knowledge/Medicine_and_healthcare/Pharmaceutical_medicine/Chemoproteomics/ (accessed 2026-03-16).
National Center for Biotechnology Information. Protein-Protein Interaction Detection: Methods and Analysis. https://pmc.ncbi.nlm.nih.gov/articles/PMC3947875/ (accessed 2026-03-16).
Klein, Christopher J.; Benarroch, Eduardo E. Epigenetic regulation: Basic concepts and relevance to neurologic disease. Neurology. https://www.neurology.org/doi/10.1212/WNL.0000000000000440 (accessed 2026-03-17).
National Center for Biotechnology Information. Alzheimer’s Disease: Experimental Models and Reality.https://pmc.ncbi.nlm.nih.gov/articles/PMC5253109/ (accessed 2026-03-17)